Prophylactic mastectomies
Prophylactic mastectomy is the preventive removal of the breast. It is considered for women who have a high risk of developing breast cancer. It is almost always associated with immediate reconstruction.
Book an appointment
La recherche de mutations génétiques constitutionnelles
Dr Anne Vincent Salomon
Anatomopathologiste et chef de service à l’institut Curie
Mutation génétique et chirurgie prophylactique
Dr Jenny-Claude Millochau
Chirurgie cancérologique et reconstructrice
Sur-risque de cancer du sein et chirurgie prophylactique
Dr Claude Nos
Chirurgie cancérologique et reconstructrice
Who are the women at risk?
These are women at very high risk of breast cancer:
- Women who have a known mutation. The best known are those of the BRCA1 and BRCA2 genes, but also women with PALB2, TP53, CDH1, PTEN, or STK11 mutations.
- Women with a family history that strongly suggests a genetic mutation because of multiple breast cancers, even if no mutation could be identified in the family.
- Genetics is a rapidly evolving science. The BRCA1 and 2 genes are the best known, but many other genes involved in cell repair are now identified. Thus, a patient who has no genomic mutation found during research done in 2010 may have a mutation discovered in 2025…
Monitoring or prophylactic mastectomy?
Women at high risk of breast cancer are subject to close supervision (INCa recommendations April 2017) : consultation every 6 months, yearly imaging monitoring (MRI, mammography, +/- ultrasound) with biopsy at the slightest doubt… This “close supervision” allows for early diagnosis and treatment of a possible cancerous lesion, but does not prevent its occurrence.
When the risk is very high, as in the case of women with a BRCA1 or BRCA2 genetic mutation, a prophylactic mastectomy is sometimes requested by the patient. This is the only effective way to prevent breast cancer today. The risk after bilateral mastectomy gets very low: it is not zero, but it drops to less than 5% (compared to 40 to 75% in the case of a confirmed mutation).
If the mutation concerns the BRCA1 gene, prophylactic mastectomy can be considered from the age of 30, because there is a risk of developing breast cancer at a very young age.
If the mutation affects the BRCA2 gene, the risk is somewhat lower. Prophylactic mastectomy can also be considered from the age of 30, the decision being modulated with the age of occurrence of cancers in the family.
Prophylactic mastectomy: a difficult decision
Advances in breast cancer surgery have allowed cancer patients to avoid mastectomy (removal of the breast) in many cases. Today, the breast is preserved in over 70% of cases. Paradoxically, in the context of prophylactic mastectomy, women who are not ill and who are rather young will ask for the removal of their breasts.
For some, the choice, as difficult as it may be, is clearly argued: they have a proven genetic mutation (BRCA1 or BRCA2 gene mutation) or their history suggests a significant risk of developing cancer and they are not ready to accept this risk.
For others, the decision is more difficult, particularly for women who do not carry an identified mutation and whose family history strongly suggests a genetic predisposition. Some patients may consider mastectomy, based on a personal risk that is difficult to assess with current knowledge.
Medical and psychological support for prophylactic mastectomy: decision support
The decision must be made after careful consideration and consultation with the various specialists involved. This decision is never an urgent one and is very well supervised:
The consultation with the oncogeneticist makes it possible to quantify the risk of developing breast cancer. He or she can assess a “risk” even if the mutation is not diagnosed.
The consultation with the surgeon and the gynecologist allows for the consideration of all solutions: close monitoring (once or twice a year) with ultrasound, mammography and MRI, or a prophylactic mastectomy.
Prophylactic surgery of the ovaries and fallopian tubes is systematically proposed in cases of high risk.
Psychological support is offered to women who undertake this procedure, before any decision is made. Prophylactic mastectomy often has a significant psychological impact that is difficult to anticipate before the operation. A woman may be relieved to know that she can significantly reduce this risk at the cost of a mastectomy. However, once the risk is removed, she may find it difficult to tolerate reconstructed breasts when she was not ill and to accept a result that does not satisfy her.
Reconstruction after prophylactic mastectomy
The preoperative consultation with a specialized surgeon allows to discuss the different possible reconstruction techniques, to evaluate the results that can be expected and to consider the complications, which are always possible and all the more difficult to bear since it is a preventive surgery.
The mastectomy preserves the areola and the nipple and the reconstruction is performed in the same operation, most often with a prosthesis, more rarely with a flap (i.e. using the patient’s own tissue). The choice of size, shape and surface of the prostheses is discussed in consultation.
Prosthesis reconstruction after prophylactic mastectomy: Before / After
Below are a few photos that give an overview of the results of breast reconstruction with prostheses after a prophylactic mastectomy.
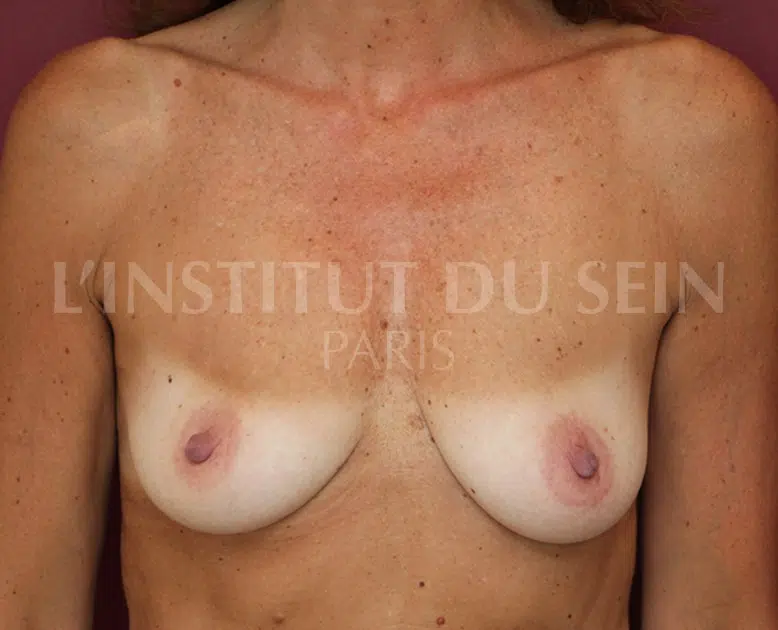

1.1 Bilateral prophylactic mastectomy and immediate reconstruction with prostheses.


1.2 Bilateral prophylactic mastectomy and immediate reconstruction with prostheses.
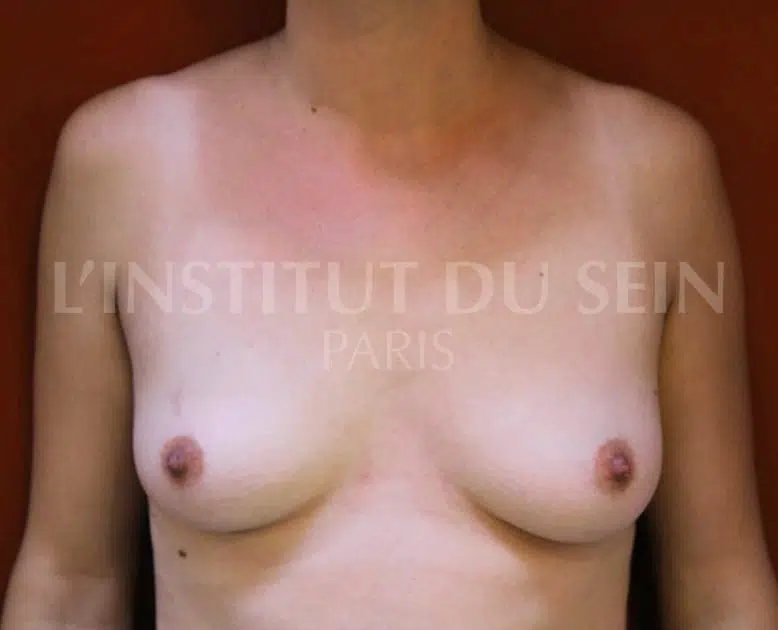
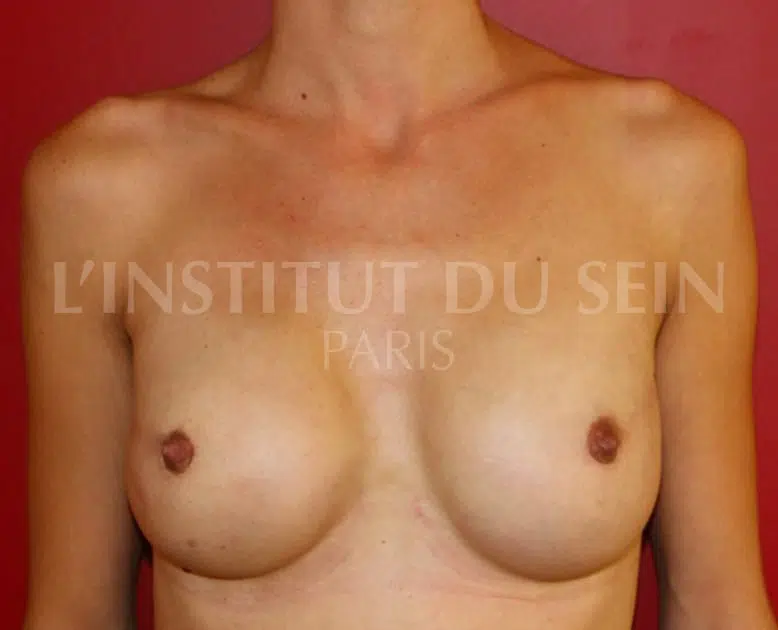
2. Bilateral prophylactic mastectomy and immediate reconstruction with prostheses.


3. Bilateral prophylactic mastectomy and immediate reconstruction with prostheses.
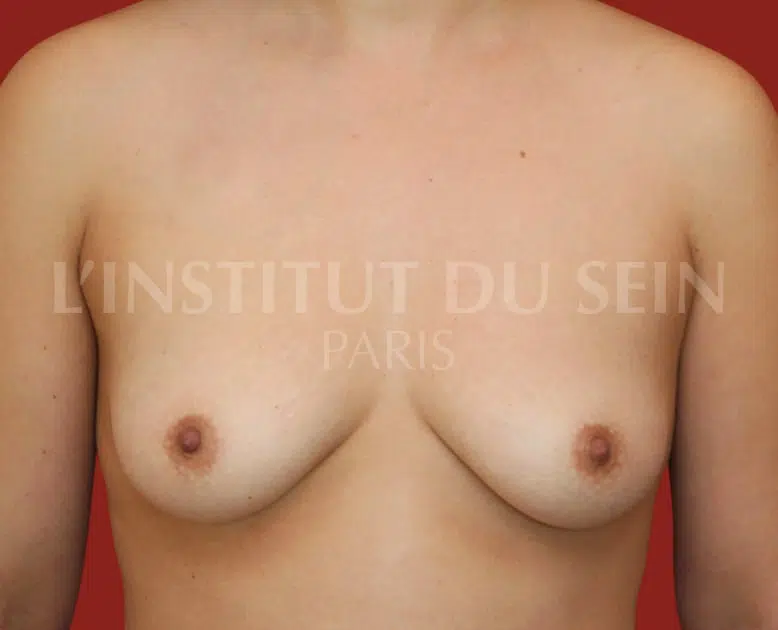
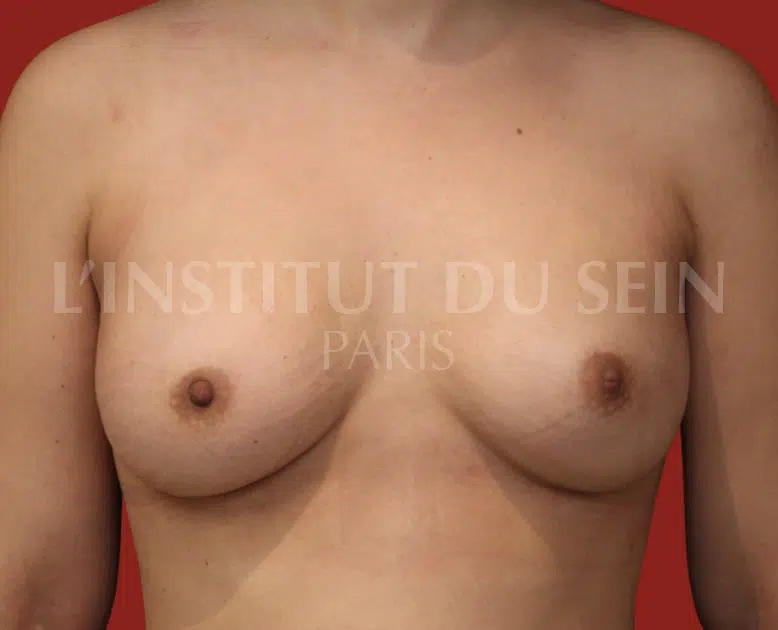
4. Bilateral prophylactic mastectomy and immediate reconstruction with prostheses.
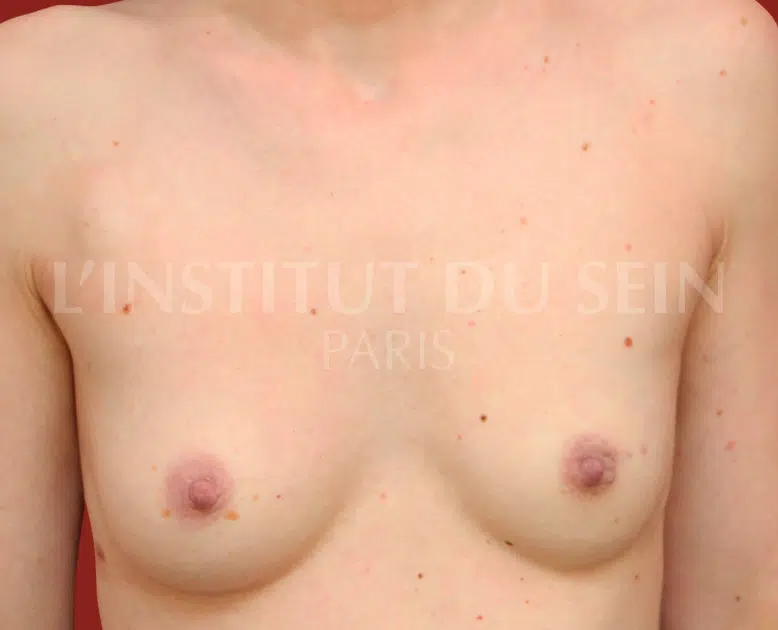

5. Left breast cancer: Total mastectomy and right prophylactic mastectomy. Immediate bilateral breast reconstruction with prostheses.
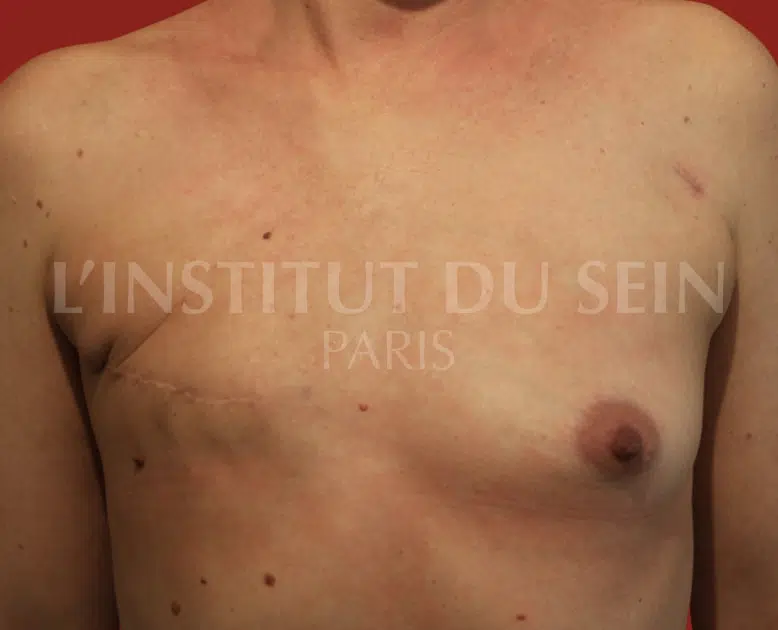
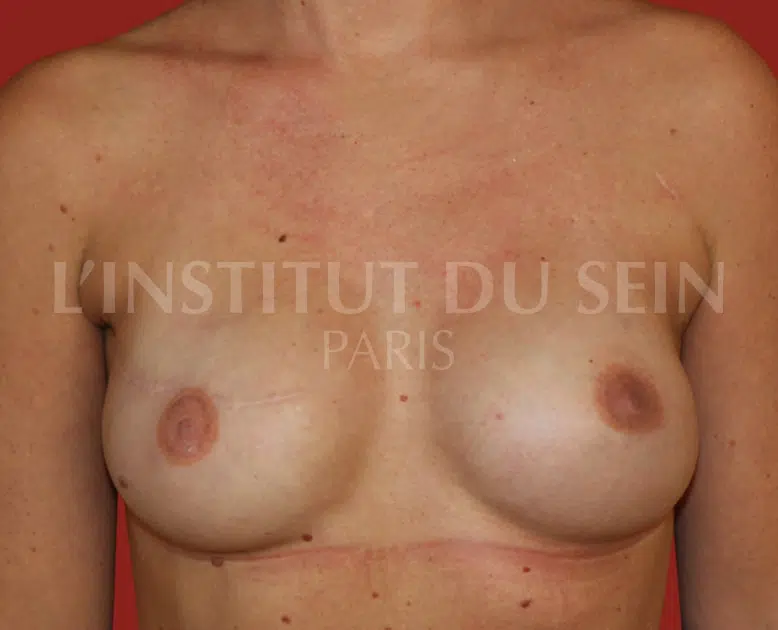
6. Left prophylactic mastectomy and bilateral reconstruction with prostheses.
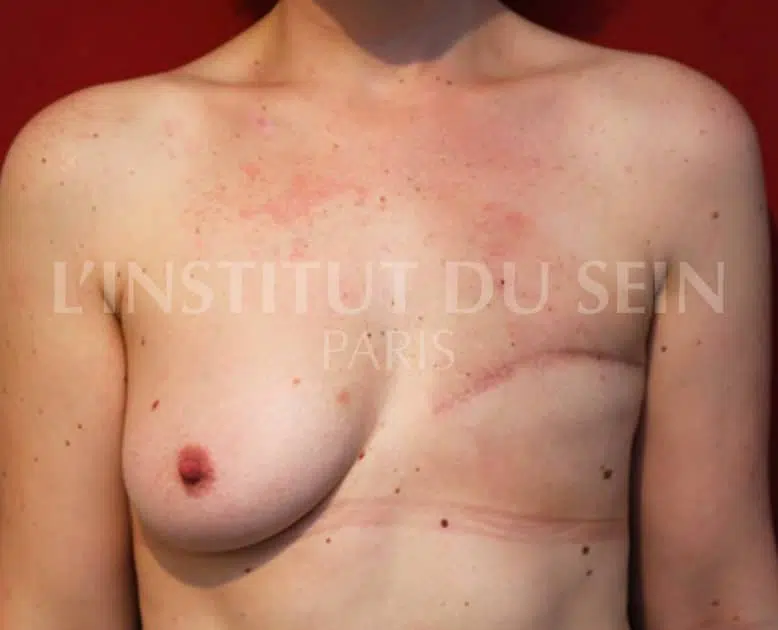

7. Left mastectomy. Reconstruction by prosthesis. Right prophylactic mastectomy, reconstruction by prosthesis.
Prophylactic adnexectomy
Prophylactic adnexectomy is the removal of the ovaries and tubes. It is recommended for patients with a BRCA1, BRCA2, PALB2, RAD51C, RAD51D, MMR mutation or a family history of ovarian cancer. It is performed from the age of 40 (it can be postponed to 45 in case of BRCA2 mutation). The benefit of adnexectomy is twofold. It significantly reduces the risk of ovarian cancer (which is between 20 and 40%, compared to 0.001% in non-mutated women). Adnexectomy has also been shown to reduce the risk of breast cancer.




Laissez votre commentaire